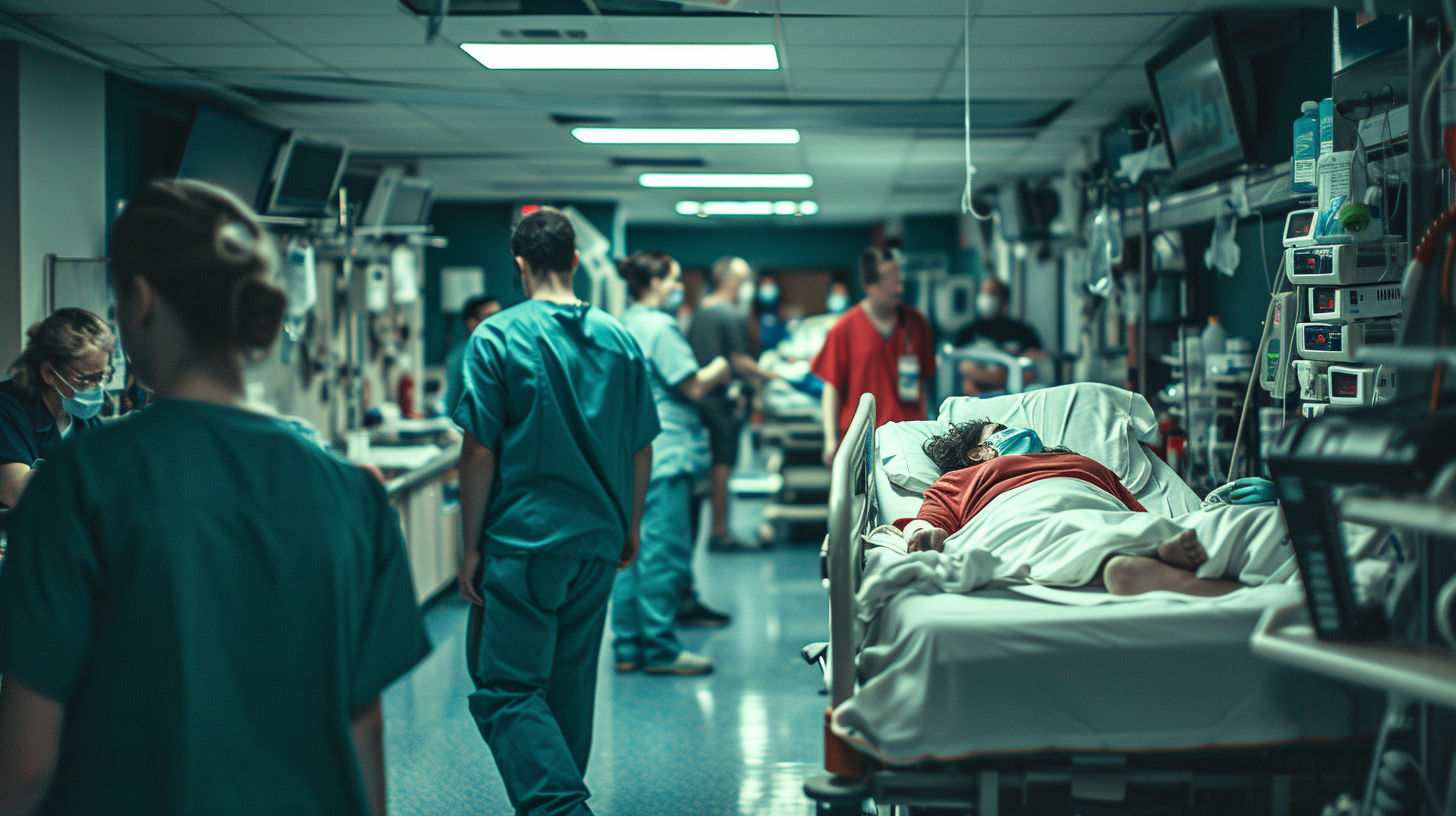
Hospital emergency rooms (ER) are busy places.
Yet, many administrators and bean counters are more interested in metrics than medicine. Under the guise of monitoring productivity, many hospitals and practice groups require emergency physicians to see an unrealistic number of patients per hour. In fact, the metric of patients per hour is a major driver for some physician payment systems.
The problem with this type of setup of measuring a patient per hour doesn’t take into account the complexity or acuity of individual patients. Sure, there are times when a hospital ER is full of patients with minor injuries or conditions. When that happens, it’s easy to see them treat a large number of patients in a relatively short span of time.
Do ER Physicians Have Enough Time for Complex Cases?
But what about those other occasions when there are multiple patients with complex conditions, like traumatic injuries, potential strokes, or heart attacks? Do you think it’s possible for an ER physician to assess and appropriately treat those conditions in just a few minutes? I don’t think so.
In the ever-present effort to see more patients in less time, hospitals have supplemented non-physician emergency room staffing, including nurse practitioners and physician assistants.
The Role of Non-Physician Staff in ERs
These members of the healthcare team used to be called mid-level providers, to indicate that they had more training than, for example, a registered nurse but less than a doctor. Some states allow nurse practitioners and physician assistants to practice nearly or completely independent of medical supervision by a physician. That’s not the case in Texas, by the way, where their care still requires physician supervision.
Inappropriate Discharges: A Growing Concern
We’ve handled numerous cases where patients were inappropriately discharged from the hospital emergency room by a nurse practitioner or physician assistant, when the patient wasn’t even evaluated by a physician.
That happened to a man in his late 30s whose wife took him to the hospital while he was having stroke symptoms. The entire time he was in the ER, he wasn’t seen by a physician.
Ensuring Proper Care: Questions to Ask Before Discharge
If you’re in a situation where you’re being pressured to leave the hospital or feel like a discharge is being prematurely pushed, here are the 2 questions to ask:
Question 1: Who’s my attending physician, and is he or she writing the discharge order? If you haven’t seen your attending physician, ask for an evaluation before you’re discharged.
Question 2: Can I have a second opinion? Then explain how your condition has improved during your stay. Be careful to describe all of your signs and symptoms, including when they developed.
Advocating for Patient Safety
In many other situations, we’ve had clients who felt like they were being pushed out the hospital door even though they had the same symptoms that brought them to the ER in the first place, or even worse.
For instance, we represented a client who slipped and fell on ice, lacerating her head in the process. Over the course of her emergency room encounter at a northeast Houston hospital, her condition deteriorated to the point that she couldn’t move her arms. Yet, there was an order to discharge her, which the nurses executed even though they had to lift her up and position her in a wheelchair and then physically lift her up and put her in a car to be driven home.
Seeking Justice for Medical Malpractice
If you’ve been seriously injured because of poor care in the emergency room in Texas, then contact a top-rated, experienced Texas medical malpractice lawyer for a free consultation about your potential case.
These legal professionals can help you navigate the complexities of medical malpractice claims, ensuring that your rights are protected and seeking justice for the harm you may have endured. Your well-being is paramount, and holding negligent parties accountable is crucial for improving overall healthcare standards.
Remember, your health and safety should always be a priority, and understanding your rights as a patient is an essential step in ensuring the highest quality of medical care. If you believe you’ve been a victim of medical malpractice, don’t hesitate to seek the guidance of a qualified attorney who can provide the support and advocacy you need.